Ready or Not 2026: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism
As TFAH marks its 25th anniversary, this annual report assesses the nation’s public health emergency preparedness at a pivotal moment. In 2025, the country faced the most severe flu season in nearly a decade, rising measles outbreaks, continued H5N1 avian influenza activity, and a growing number of extreme weather events—all while the federal systems built over decades to help states prepare for and respond to emergencies came under significant strain.
Ready or Not 2026: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism evaluates the nation’s readiness for public health emergencies through 10 indicators of state preparedness, including healthcare workforce mobility, state public health funding, laboratory surge planning, access to paid sick leave, and community water system safety.
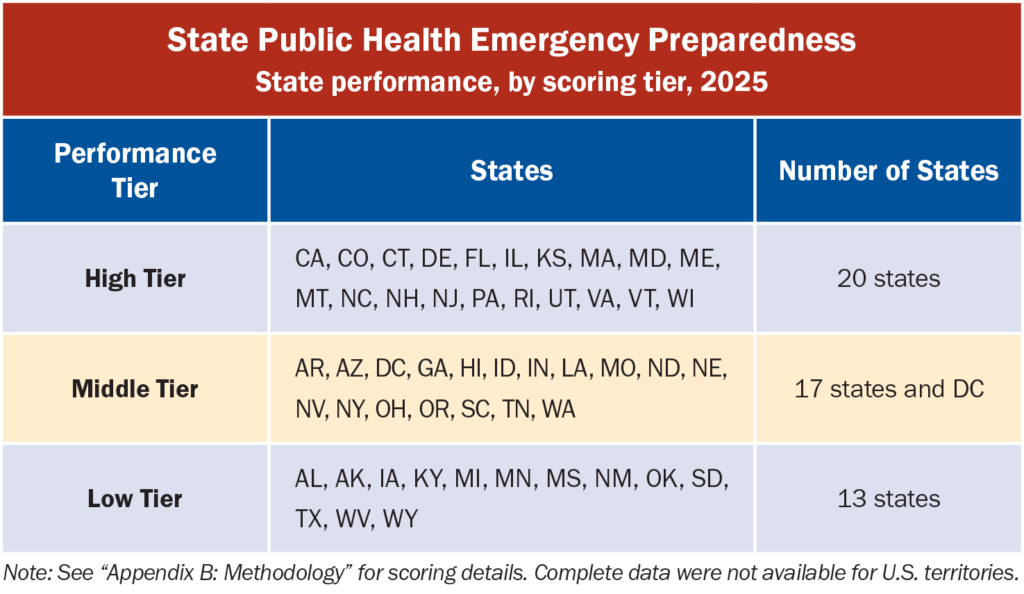
The report also places states and the District of Columbia into three performance tiers: 20 states in the high-performance tier, 17 states and the District of Columbia in the middle-performance tier, and 13 states in the low-performance tier.
2025: A Year of Compounding Public Health Emergencies
During 2025, the nation faced a series of significant public health emergencies, including the most severe influenza season in nearly a decade, the highest number of measles cases since 1991, continued H5N1 avian influenza cases, and extreme weather events such as wildfires, hurricanes, and extreme heat.
These overlapping threats underscore the urgent need for sustained investment in public health infrastructure and preparedness—both essential to protecting the public’s health, economic security, and national resilience.
Special Feature: Preparedness at Risk
This year’s report includes a special feature examining how federal workforce reductions and funding instability could weaken preparedness nationwide.
Reductions in federal health agency staffing, public health grant terminations, and sustained funding uncertainty have created significant challenges for maintaining the systems needed to respond effectively to emergencies. As the report documents, these changes put at risk the preparedness infrastructure that decades of bipartisan federal investment helped build.
Recommendations for Action
The report provides federal, state, and local policymakers and health officials with benchmarks and policy recommendations to help strengthen preparedness nationwide.
“The nation faced the most severe flu season in nearly a decade, the highest annual measles case count since 1991, and devastating weather-related emergencies, even as federal public health funding, staffing, and operational support were destabilized,” said Dr. J. Nadine Gracia, President and CEO of TFAH. “These challenges make clear that emergency preparedness cannot rely on a patchwork of limited and unpredictable resources. Effective readiness requires strong federal leadership, stable investment, and coordinated action across states and communities, especially as the United States prepares to host matches during the 2026 World Cup.”
Overall Findings
Overall, the report finds that national preparedness depends not only on state-level capacity, but also on strong and stable federal systems, sustained intergovernmental coordination, and long-term investment in public health infrastructure.
Areas of strong performance include:
- Nurse Licensure Compact: As of early 2026, 41 states have adopted the Nurse Licensure Compact, improving states’ ability to rapidly mobilize nursing personnel across state lines during emergencies.
- Public Health and Emergency Management Accreditation: Most states are accredited by the Public Health Accreditation Board and/or the Emergency Management Accreditation Program, strengthening coordination, accountability, and emergency response capabilities.
- Public Health Laboratory Surge Capacity: Nearly every state has a written plan in place to expand laboratory testing capacity during a prolonged public health emergency.
- Community Water System Safety: Most residents continue to receive water from community water systems that meet health-based safety standards, though important risks and inequities remain.
Areas for improvement include:
- Federal Funding and Workforce Stability: Uncertainty and reductions in federal public health funding and staffing have introduced significant risks to long-term preparedness capacity, with effects likely to compound over time.
- State Public Health Funding: While a majority of states maintained or increased public health funding in FY 2025, at least 12 states reduced funding—a concerning trend at a moment of heightened federal uncertainty.
- Paid Sick Leave: Access to paid sick leave varies widely across U.S. regions—from 98 percent of workers in Pacific states to 67 percent in East South Central states—and gaps are most concentrated among low-wage, part-time, and service-sector workers. Paid sick leave reduces disease transmission, supports business continuity, and is increasingly recognized by employers as an important part of preparedness infrastructure.
- Flu Vaccination Rates: Flu vaccination coverage remains too low in many states, weakening a key foundation of outbreak and pandemic preparedness.
- Hospital Patient Safety: In fall 2025, only 27 percent of graded hospitals earned an “A” from the Leapfrog Hospital Safety Grade, with wide variation across states. Strong patient safety performance can help hospitals maintain care quality and manage surge capacity during emergencies.
- Avoidable Mortality: Significant disparities persist across states and population groups, reflecting ongoing gaps in healthcare access, public health capacity, and underlying community conditions.
- Infrastructure and Environmental Risks: Aging infrastructure and increasing climate- and weather-related threats pose growing challenges to preparedness.
Recommendations for Improving Emergency Preparedness:
- Provide stable, flexible, and sufficient funding for public health preparedness, workforce, and data modernization to help ensure every state has the systems needed to protect residents.
- Restore the federal public health workforce and capabilities reduced in 2025.
- Reauthorize the Pandemic and All-Hazards Preparedness Act.
- Strengthen outbreak and pandemic readiness by supporting immunization, public health surveillance, and antimicrobial resistance efforts.
- All levels of government should adopt strategies and accountability metrics to incorporate community resilience and health equity into preparedness.
- Accelerate development, stockpiling, and distribution of vaccines, therapeutics, diagnostics, and other medical countermeasures.
- Bolster healthcare system readiness, including cross-state credentialing and investment in Health Care Readiness programs.
- Expand preparedness for extreme weather and environmental health threats.

