Ready or Not 2023: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism
This 20th edition of TFAH’s Ready or Not report measures states' emergency preparedness and makes recommendations about how to strengthen the nation's public health system. Sustained investment in public health infrastructure and preparedness is needed to protect lives during disease outbreaks and natural disasters.
(March 23, 2023) Ready or Not 2023: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism measures states’ readiness to respond to a spectrum of health emergencies and to provide ongoing public health services. The report gives federal and state health officials and policymakers actionable data and recommends policies to improve the nation’s emergency preparedness at a time when health emergencies are increasing. During 2022, the U.S. surpassed 1 million deaths due to COVID-19 and saw decreasing rates of routine vaccinations and increasing prevalence of health misinformation. In addition, the past year was the eighth consecutive year the U.S. experienced 10 or more billion-dollar weather-related disasters.
The report tiers states and the District of Columbia into three performance levels for health emergency preparedness: high, middle, and low. This year’s report placed 19 states and DC in the high-performance tier, 16 states in the middle performance tier, and 15 states in the low performance tier.
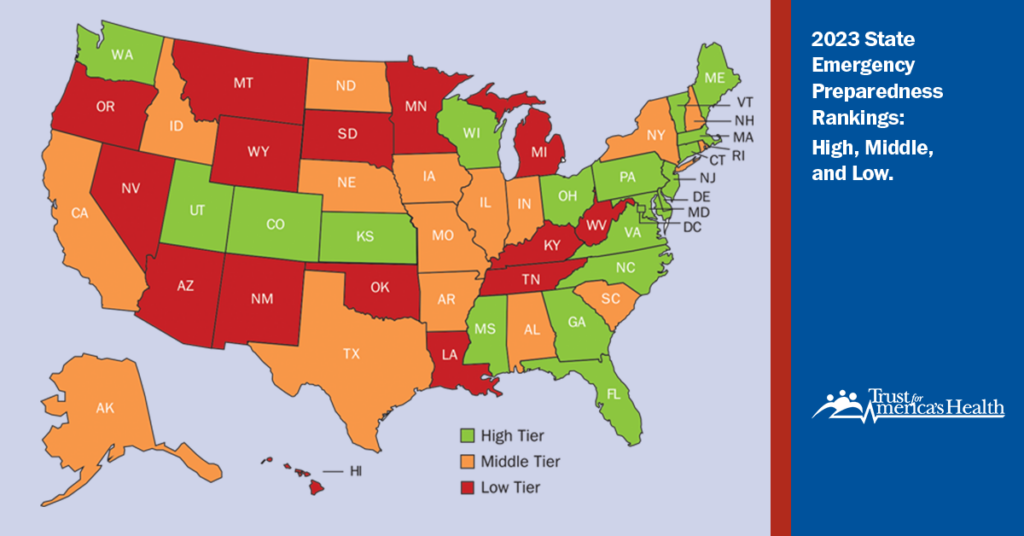
States' Performance by Tiers
| Performance Tier | States | Number of States |
| High Tier | CO, CT, DC, DE, FL, GA, KS, ME, MD, MA, MS, NJ, NC, OH, PA, UT, VT, VA, WA, WI | 19 states |
| Middle Tier | AK, AL, AR, CA, IA, ID, IL, IN, MO, ND, NE, NH, NY, RI, SC, TX | 16 states |
| Low Tier | AZ, HI, KY, LA, MI, MN, MT, NM, NV, OK, OR, SD, TN, WV, WY
|
15 states |
The report’s findings showed both areas of strength within the nation’s public health system and areas that need attention
Areas of strong performance include:
- A majority of states have made preparations to expand healthcare and public health laboratory capacity in an emergency.
- Most states are accredited in the areas of public health or emergency management. Some states are accredited in both.
- Most U.S. residents who received their household water through a community water system had access to safe water. However recent water system failures in Jackson, Mississippi and Newark, New Jersey demonstrate the importance of continued attention to the integrity of municipal water systems.
Areas that need attention include:
- Too few people were vaccinated against seasonal flu last year despite significant improvement in flu vaccination rates in recent years. During the 2021-2022 flu season, 51 percent of Americans ages 6 months or older received a flu vaccine, well short of the 70 percent goal established by Healthy People 2030.
- Only about half the U.S. population is served by a comprehensive public health system. Comprehensive public health systems ensure that necessary health services are available to all residents.
- Only 26 percent of hospitals in states, on average, earned a top-quality patient safety grade in 2022. Hospital safety scores measure performance on such issues as healthcare-associated infection rates, intensive-care capacity, and an overall culture of error prevention.
“Increased and sustained investment in public health infrastructure, emergency preparedness, and health equity will save lives,” said J. Nadine Gracia, M.D., MSCE, President and CEO of Trust for America’s Health. “Federal, state, and local officials as well as leaders in the healthcare and business sectors should use our findings to identify and address gaps in public health preparedness. Neglecting to do so will mean that the country will not be as prepared as it needs to be for the next public health emergency.”
The report contains recommendations for policy actions that would create a stronger public health system at all levels, including:
- The Administration, Congress, and state lawmakers should modernize public health infrastructure, including by investing $4.5 billion annually to support foundational public health capabilities. In addition, Congress should continue to increase funding for the Public Health Emergency Preparedness cooperative agreement and public health data modernization to allow for earlier and more accurate detection of emerging health threats.
- Policymakers at all levels should act to protect and strengthen public health authorities and should prioritize rebuilding trust in public health agencies and leaders.
- Congress and state legislatures should invest in effective public health communications, including countering misinformation.
- Congress and states should ensure first-dollar coverage for all recommended vaccines under commercial insurance and for uninsured people. States should minimize vaccine exemptions for school children, and healthcare facilities should increase rates of vaccination for healthcare workers.
- Congress and states should provide job-protected paid leave for employees due to illness or family caregiving demands.
- Congress and states should invest in policies and capacity to address the social determinants of health such as secure housing, access to transportation, and access to healthy food.
- Congress should fund the entire medical countermeasures (MCM) enterprise, including the distribution and dispensing of MCMs. Congress should also create incentives for new products to prevent and fight antibiotic-resistant infections.
- Congress and states should strengthen readiness for climate change, extreme weather, and environmental health threats.
Read the full report

