U.S. Obesity Rates Reach Historic Highs – Racial, Ethnic, Gender and Geographic Disparities Continue to Persist
Report calls for sugary drink taxes, expanded SNAP and WIC Nutrition support programs and a built environment that encourages physical activity to help address health crisis.
Executive Summary
Obesity is a growing epidemic in the United States – and has been for decades. Currently, about one in three Americans of all ages – or more than 100 million people – have obesity.
This report based in part on newly released data from the Centers for Disease Control and Prevention’s Behavioral Risk Factor Surveillance System (BRFSS), and analysis by TFAH, provides an annual snapshot of obesity rates nationwide.
Obesity has serious health consequences including increased risk for type 2 diabetes, high blood pressure, stroke and many types of cancers. Obesity is estimated to increase national healthcare spending by $149 billion annually (about half of which is paid for by Medicare and Medicaid) and being overweight or obese is the most common reason young adults are ineligible for military service.
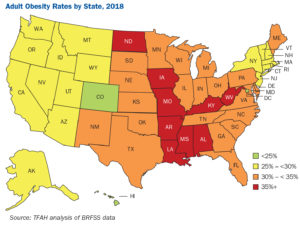
Nine U.S. states had adult obesity rates at or above 35 percent in 2018, up from seven states at that level in 2017, an historic level of obesity in the U.S. The nine are: Alabama, Arkansas, Iowa, Kentucky, Louisiana, Mississippi, Missouri, North Dakota and West Virginia.
Obesity rates vary considerably between states with Mississippi and West Virginia having the highest level of adult obesity in the nation at 39.5 percent and Colorado having the lowest rate at 23.0 percent.
- As recently as 2012, no state had an adult obesity rate over 35 percent and within the last five years (2013 and 2018) 33 states had statistically significant increases in their rates of adult obesity.
A second data source referenced in the report, the National Health and Nutrition Examination Survey (NHANES) also shows unprecedented levels of obesity in the U.S. In 2015-2016, the most recent available data, the national adult obesity rate was 39.6 percent and the national child obesity rate was 18.5 percent. Strikingly, the incidence of obesity in the U.S. has increased by 70 percent over the last 30 years for adults and by 85 percent over the same time period for children.
“These latest data shout that our national obesity crisis is getting worse,” said John Auerbach, President and CEO of Trust for America’s Health. “They tell us that almost 50 years into the upward curve of obesity rates we haven’t yet found the right mix of programs to stop the epidemic. Isolated programs and calls for life-style changes aren’t enough. Instead, our report highlights the fundamental changes that are needed in the social and economic conditions that make it challenging for people to eat healthy foods and get sufficient exercise.”
Differential Impact Amongst Minority Populations
The report highlights that obesity levels are closely tied to social and economic conditions and that individuals with lower incomes are more at risk. People of color, who are more likely to live in neighborhoods with few options for healthy foods and physical activity, and, are the target of widespread marketing of unhealthy foods, are also at elevated risk.
As of 2015-2016, nearly half of Latino (47 percent) and Black adults (46.8) had obesity while adult obesity rates among White and Asian adults were 37.9 percent and 12.7 percent respectively. Incidence of childhood obesity was highest amongst Latino children at 25.8 percent while 22 percent of Black children had obesity, 14 percent of White children had obesity and 11 percent of Asian children had obesity.
What Could Work?
While the obesity rates are alarming, there are new data offering the promise of policies that combat the epidemic, namely promoting healthier food for children through revamped WIC food packages and fostering behavior change through taxes on sugary drinks.
- Obesity rates for children enrolled in WIC (Special Supplemental Nutrition Program for Women, Infants and Children) continue to decline, from 15.9 percent in 2010 to 13.9 percent in 2016. In 2009, the USDA updated WIC food packages to more closely meet recommended national dietary guidelines including the addition of more fruits, vegetables and whole grains and reduced fat levels in milk and infant formula. A Los Angeles County study published this year found that 4 year-olds who had received the revised WIC food package since birth had reduced risk for obesity.
- A number of US. cities and the Navajo Nation have passed local taxes on sugary drinks that are showing promise as a means to change consumers’ beverage habits. Studies of a 2014 1-cent per ounce tax in Berkeley, California found decreased consumption of sugary drinks there. Likewise, a 2019 study of a 1.5 cent per ounce tax in Philadelphia, Pennsylvania found that the consumption of sugary drinks decreased significantly after the tax was imposed.
Recommendations for Policy Action
The report includes 31 recommendations for policy action by federal, state and local government, across several sectors, designed to improve access to nutritious foods and provide safe opportunities for physical activity, while minimizing harmful marketing and advertising tactics. All of the report’s recommendations are grounded in two key principles: the complexity of the obesity crisis requires multi-sector solutions and a systems approach, and, interventions should focus on communities with the highest levels of obesity first as a matter of health equity and because such interventions offer the best opportunity to impact the problem.
Among the report’s recommendations for policies to address the obesity crisis are:
- Expand the Special Supplemental Nutrition Program for Women, Infants and Children (WIC) to age 6 for children and for two years postpartum for mothers. Fully fund the WIC Breastfeeding Peer Counseling Program.
- Increase the price of sugary drinks through excise taxes and use the revenue to address health and socioeconomic disparities.
- Ensure that CDC has enough funding to grant every state appropriate funding to implement evidence-based obesity prevention strategies (currently, CDC only has enough funding to work with 16 states).
- Make it more difficult to market unhealthy food to children by ending federal tax loopholes and business costs deductions related to the advertising of such foods to young audiences.
- Fully fund the student Support and Academic Enrichment program and other federal programs that support student physical education.
- Encourage safe physical activity by funding Safe Routes to Schools (SRTS), Complete Streets, Vision Zero and other pedestrian safety initiatives through federal transportation and infrastructure funding.
- Ensure that anti-hunger and nutrition-assistance programs, like the Supplemental Nutrition Assistance Program (SNAP), WIC and others follow the Dietary Guidelines for Americans and make access to nutritious food a core program tenet.
- Strengthen and expand school nutrition programs beyond federal standards to include universal meals, flexible breakfasts and eliminate all unhealthy food marketing to students.
- Enforce existing laws that direct most health insurers to cover obesity-related preventive services at no-cost sharing to patients.
- Cover evidence-based comprehensive pediatric weight management programs and services in Medicaid.