Staffing Up: Public Health Workforce Must Grow to Provide Basic Public Health for All Americans
Public health budget and staffing cuts have weakened America’s health security and increased Americans’ vulnerability to emerging infectious and chronic diseases.
State and local governmental public health departments are essential to maintaining the security, safety, and prosperity of local communities, yet they are consistently underfunded. A recent analysis conducted by the de Beaumont Foundation and the Public Health National Center for Innovations (PHNCI) found state and local governmental public health departments have lost 15 percent of their essential staff over the last decade. These staffing cuts have been especially detrimental in the midst of the global pandemic as understaffed health departments had a limited ability to plan for and respond to emergencies like COVID-19 and struggle to meet the daily health security needs of their communities.
The issue brief, Staffing Up: Workforce Levels Needed to Provide Basic Public Health Services for All Americans, found that nationally state and local governmental public health departments need an 80 percent increase in their workforce (80,000 additional full-time employees) to provide an adequate infrastructure and a minimum set of public health services to the nation (See Figure 1). Specifically, due to existing staffing shortages local health departments need to add approximately 54,00 full-time employees, and state departments need to add 26,000 full-time employees across differing levels of categories and areas of expertise. (See Figure 4).
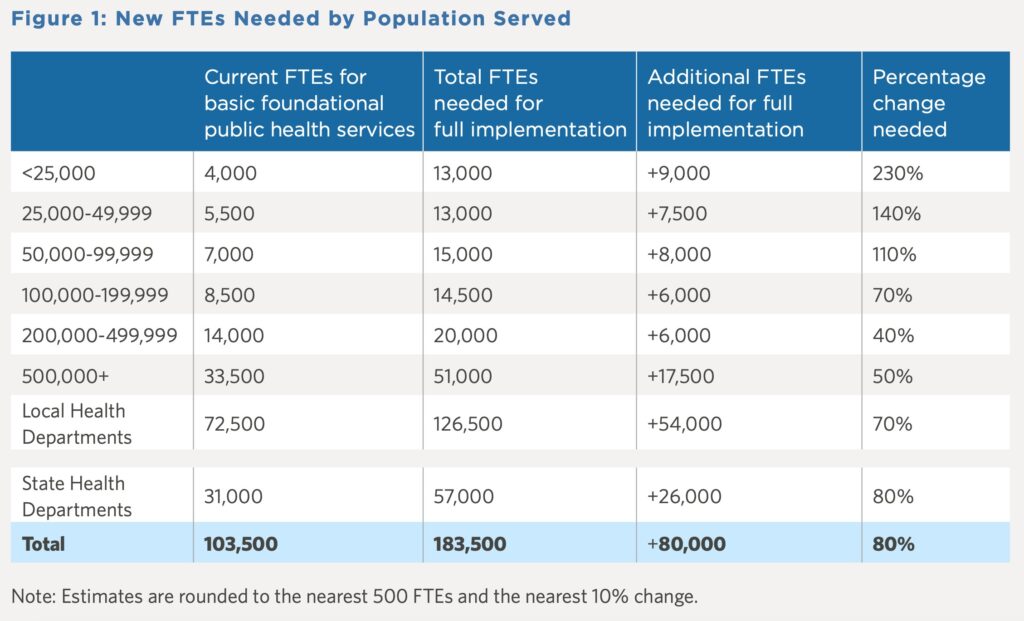
Source: Staffing Up: Workforce Levels Needed to Provide Basic Public Health Services for All Americans
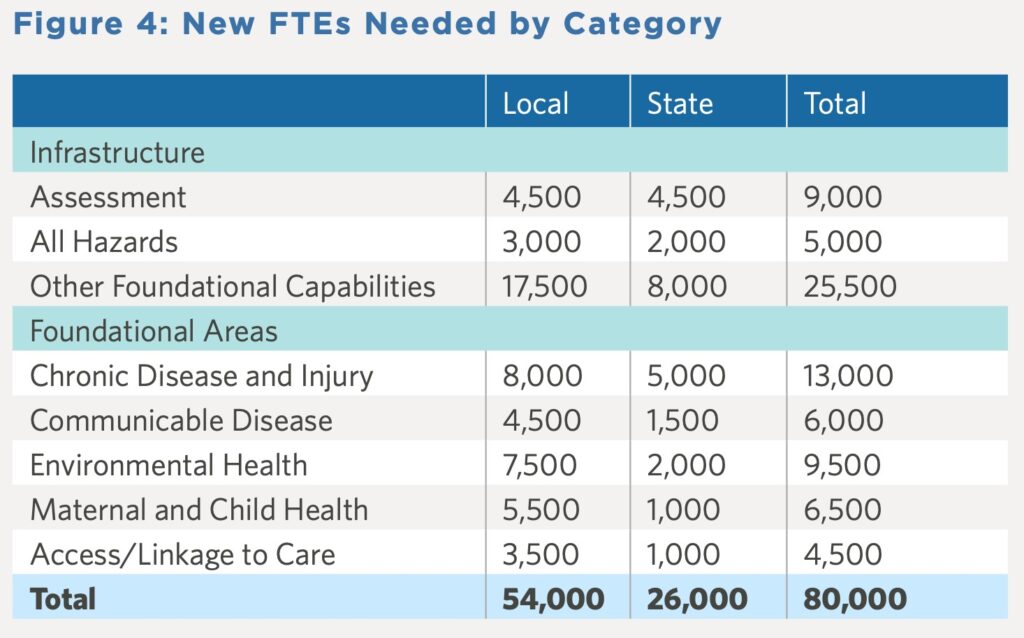
Source: Staffing Up: Workforce Levels Needed to Provide Basic Public Health Services for All Americans
This chronic underfunding of the public health system was a key contributing factor in the nation’s unprepared response to the COVID-19 pandemic, according to TFAH’s report, The Impact of Chronic Underfunding on America’s Public Health System: Trends, Risks, and Recommendations, 2021. The report highlights how the underfunding of core public health programs – resulting in under-resourced, understaffed, and overburdened health agencies – impeded the pandemic response and exacerbated its impacts. Years of underfunding core public health programs created the situation in which local health departments were fighting a 21st century pandemic with 20th century tools and has made the nation less resilient, the report said.
To combat the growing public health crisis, and emerge better prepared for future public health emergencies, the U.S. needs to adequately fund public health and disease prevention all the time, not just in response to a crisis, and it needs to address the social determinants of health. At present, the country spends about $3.8 trillion on healthcare with just 2.6 percent of that spending directed toward public health and prevention.
Investment to ensure foundational capabilities is key. (See Figure 5).
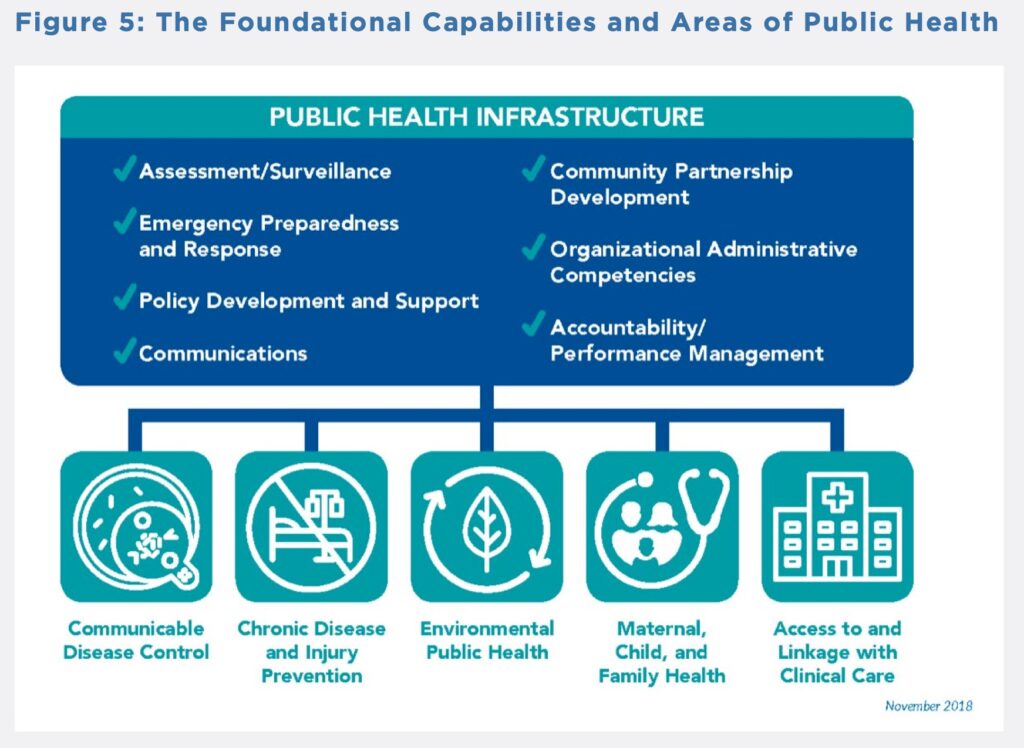
Source: Staffing Up: Workforce Levels Needed to Provide Basic Public Health Services for All Americans
TFAH’s public health funding report calls for a $4.5 billion annual investment in the nation’s core public health capabilities, and includes four priorities for policy action:
- Substantially increase core funding to strengthen the public health system, including by building and supporting the workforce, modernizing the system’s data tools and increasing its surveillance capacities.
- Strengthen public health emergency preparedness, including within the healthcare system.
- Safeguard and improve Americans’ health by investing in chronic disease prevention and the prevention of substance misuse and suicide.
- Take steps to advance health equity by combating the impacts of racism and addressing the social determinants that lead to poor health.