State Category: South Carolina
COVID-19, Five Years Later: Will We Heed the Public Health Lessons?
(Washington, DC – April 17, 2025) – March 2025 marked the five-year anniversary of the declaration of COVID-19 as a pandemic. This milestone offers an opportunity to reflect on the heroic work of healthcare providers and the public health workforce in limiting the pandemic’s impact on Americans’ health. Public health professionals across the country worked tirelessly on the frontlines—often facing unprecedented challenges, personal risk, and even harassment—while providing essential services such as contact tracing, coordinating testing, distributing and administering vaccines, and offering life-saving guidance to communities. Their dedication and expertise were vital to the national response and demonstrated the indispensable role of public health infrastructure in protecting American lives during a crisis.
It is also a time to remember the pandemic’s toll in illness, lives lost, and social and economic disruption. Finally, this anniversary presents an opportunity to consider what can be learned from the pandemic and how those lessons can be applied to protect the nation’s health and economic security during future emergencies.
According to the World Health Organization, COVID-19 deaths worldwide have exceeded seven million. In the U.S., at least 1.2 million people have died from COVID-19, according to the Centers for Disease Control and Prevention (CDC).
While the public health emergency has ended, COVID-19 infections are still occurring, albeit at a much lower rate. Staying up to date with vaccination remains one of the most effective tools to prevent severe illness, hospitalization, and death from COVID-19—especially when combined with other preventive measures, as appropriate, based on current community transmission levels and individual risk factors.
We continue to face numerous public health risks that demand action, including a multi-state measles outbreak, a tuberculosis outbreak, bird flu, and environmental threats. All of this is happening as federal budget cuts threaten the capacity of federal, state, and local public health departments to respond to emergencies, while workforce reductions risk the loss of sorely needed public health expertise and experience.
COVID-19 Funding Ended the Emergency and Strengthened Public Health Readiness
The COVID-19 pandemic demanded an unprecedented public health response, including funding to modernize the nation’s public health infrastructure and expand its workforce. New funding for CDC’s Data Modernization Program increased the number of healthcare facilities using electronic case reporting (eCR) to report infectious disease cases to public health agencies—from 153 in January 2020 to over 50,000 in February 2025. eCR enables real-time disease tracking, allowing for a faster response to outbreaks. Additional examples include the Public Health Infrastructure Grant, which provides funding to health departments nationwide to support innovative investments in workforce, systems, and services tailored to meet their communities’ specific health priorities and challenges; the establishment of a new Center for Forecasting and Outbreak Analytics at the CDC to model and predict outbreak trends; and the expansion of CDC’s National Wastewater Surveillance System, now implemented in 46 states and the District of Columbia. These critical new capacities are at risk due to federal budget cuts.
What the Pandemic Taught Us
The lessons of the pandemic are numerous and should be applied to strengthen the public health system. Doing so would help ensure that the nation is better prepared for future risks. These lessons include:
- Protecting CDC’s mission—including its comprehensive focus on both chronic and infectious diseases—is essential, because healthier communities, particularly those with a lower burden of chronic disease, are more resilient during emergencies and recover more quickly.
- A modernized and interoperable health data infrastructure is critical for real-time disease tracking. Such systems allow healthcare and public health officials to target resources where they are needed most. The progress made in data modernization since 2020 must be sustained.
- Public health and healthcare readiness, along with surge capacity, are critical in an emergency. Healthcare workforce shortages during the acute phases of the pandemic placed tremendous strain on the system’s ability to manage the surge of patients. The emergency readiness of the healthcare delivery system must be fortified. State public health laboratories were also vital in identifying cases and tracking disease spread. Most states have laboratory surge plans that helped them expand testing capacity during peaks in pandemic transmission. Telehealth was a critical platform for healthcare access during the pandemic, and reimbursement for telehealth services should be preserved.
- A strong emergency preparedness system is vital to the nation’s economic security. The COVID-19 emergency led to major economic disruptions and the largest employment loss in the U.S. since World War II. A 2023 study by a team of economists estimated that the pandemic’s impact on the U.S. economy through the end of 2023 was $14 trillion. Going forward, protecting the nation’s economy will require systems and capacities that can prevent a small number of disease cases from escalating into an outbreak—and eventually a pandemic.
- The pandemic highlighted the nation’s health and economic disparities and their impact on health outcomes during emergencies. While all communities may face health emergencies, the impacts are not felt equally. Communities with higher rates of chronic disease and underlying health conditions often experience worse outcomes—disparities rooted in systemic barriers such as income inequality, housing instability, discrimination, poor air and water quality, and gaps in healthcare access. Advancing health equity by addressing these challenges is essential to building a more resilient and prepared nation.
- The COVID-19 vaccines saved lives and reduced the severity of illness. The rapid development of the vaccines, along with an expansive system to administer them, played a critical role in the national response. According to a Commonwealth Fund study published in December 2022, COVID-19 vaccines prevented an estimated 18.5 million hospitalizations, 3.2 million deaths, and at least $1 trillion in healthcare spending in the U.S. during the first two years of the vaccination program (December 2020 through November 2022). Continued investment in vaccine development, manufacturing and distribution readiness, and other medical countermeasures is essential. mRNA vaccine technology is well-positioned to quickly produce effective vaccines against future virus variants.
- The pandemic exacerbated misinformation and disinformation about vaccine safety, particularly on social media. Vaccine education that shares accurate information and builds confidence is essential. These programs should acknowledge that some people—while open to learning more—have questions and want space to make their own decisions. Healthcare and public health officials should seek opportunities to listen and respond to individuals’ questions and concerns.
We Need to Act on the Pandemic’s Lessons
- Increased, sustained, and flexible public health funding is essential. The pattern of boom-and-bust funding cycles has left the system with serious preparedness gaps. Funding levels must be increased, and flexible funding is critical because it allows state and local health officials to quickly target and deploy resources where they are most needed. Investment in workforce growth and retention is also crucial.
- Invest in prevention to improve health and reduce healthcare spending. As a nation, we don’t spend enough on public health and prevention. Investments in these areas yield healthier communities and significant long-term savings. Typically, less than five percent of the nation’s nearly $5 trillion in annual health spending is directed to public health and prevention programs.
- Numerous sectors have a role to play in improving the public’s health. These partnerships should include public health, healthcare, educators, community–based organizations, faith leaders, the business community, and others. Strong relationships established before a crisis are central to an effective emergency response.
- Public trust in government is critical during health emergencies. The politicization of public health has weakened the system and threatens its ability to respond effectively to future crises. Upholding scientific integrity—empowering public health experts to make recommendations based on the best available information—is essential for effective emergency response. Public health authorities must be preserved, and public health agencies must be effective communicators who can clearly explain the rationale behind their guidance. Timely and transparent communication with the public is essential. Public health officials also understand the importance of maintaining strong, ongoing relationships with community organizations and leaders—not just during emergencies. A diverse public health workforce that reflects the communities it serves is also key to building trust.
Closing Thoughts
The COVID-19 pandemic was a tragic event, worsened in part by an inadequate early response. Failing to learn from the pandemic experience would only compound the tragedy. The task now facing policymakers at all levels is to invest in policies and programs that will fortify our public health system—ensuring it is fully prepared to respond quickly to future emergencies—and to restore trust in the system so it can function effectively when lives are on the line.
TFAH’s annual report series, Ready or Not: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism, identifies key strengths, areas for improvement, and recommendations to enhance the nation’s emergency preparedness.
To learn more about TFAH’s recommendations for a stronger public health system, read our 2024 report: Pathway to a Healthier America: A Blueprint for Strengthening Public Health for the Next Administration and Congress.
Statement of J. Nadine Gracia, M.D., MSCE, President and CEO, Trust for America’s Health on HHS Reorganization, Reductions in Force, and Public Health Funding Cuts
(Washington, DC – April 4, 2025) – Trust for America’s Health, a nonpartisan, nonprofit public health policy, research, and advocacy organization, is deeply concerned about the announced reorganization of federal health agencies and the broad and immediate impact of reductions in force across the U.S. Department of Health and Human Services (HHS). The impact of these actions will be heightened by the Administration’s decision to pull back public health funding already at work in states and local communities at a time when the country is experiencing infectious disease outbreaks, including measles cases in 20 jurisdictions and bird flu, rising rates of chronic disease, and devastating hurricanes, tornadoes, and wildfires.
Our serious concern is that these actions will negatively impact Americans’ health. Health that is now at greater risk due to what will be slower and less effective responses to disease outbreaks and environmental disasters, and fewer programs to surge public health and healthcare capacity in response to emergencies, ensure vaccine access, support mental health and prevent drug overdose, safeguard the food supply, and address the nation’s chronic disease crisis.
The federal government plays a critical role in securing the nation’s health through the work and expertise of numerous HHS agencies affected by these changes, such as the Centers for Disease Control and Prevention (CDC), the Food and Drug Administration (FDA), the National Institutes of Health (NIH), the Administration for Strategic Preparedness and Response (ASPR), the Substance Abuse and Mental Health Services Administration (SAMHSA), and the Office of the Assistant Secretary for Health (OASH). It also includes offices and institutes dedicated to addressing health disparities, such as my former office, the HHS Office of Minority Health whose statutory mission is to provide national leadership, resources, and coordination to improve the health of racial and ethnic minority populations and to eliminate health disparities.
Congress has long indicated its intent for federal agencies to undertake activities to protect and advance the nation’s health through authorizing and appropriations legislation. Fundamental changes impacting the Department’s ability to execute activities and programs directed by Congress should be made through a deliberate process involving Congress.
CDC’s comprehensive mission and expertise save lives. Congress has directed CDC to work on infectious and non-infectious diseases and conditions through authorizing legislation and appropriations bills. As an example, the bipartisan PREVENT Pandemics Act (P.L. 117-328) defined the obligations of the CDC Director to be “investigation, detection, identification, prevention, or control of diseases or conditions to preserve and improve public health domestically and globally and address injuries and occupational and environmental hazards.” The reported loss of CDC’s staff expertise to prevent chronic disease, birth defects, injuries, environmental hazards, and other leading causes of death and disability will directly impact the ability of the Department to carry out these important activities.
Furthermore, about 80 percent of CDC’s domestic budget goes directly to states, localities, tribal organizations, community and faith-based organizations, universities, healthcare systems, and other partners. When emergencies happen, the expertise of CDC staff and the funding and technical assistance CDC provides to state and local health departments are critical to waging an effective response. That was the case when Hurricane Helene hit North Carolina and Tennessee, during the East Palestine, Ohio train derailment, and the Los Angeles area wildfires. Cuts to CDC make every community more vulnerable to health threats and would be particularly detrimental to local public health infrastructure in rural communities and other underserved areas.
Dozens of states have estimated their funding losses based on the announced claw-back of pandemic era funding, funding intended to help states not only protect against COVID-19 infections but also build their disease detection infrastructure to protect residents during future health emergencies. The abrupt cancellation of these funds is impacting critical on-the-ground health protection activities, including bird flu testing, measles vaccinations, the electronic data systems that make the sharing of information between healthcare facilities and public health agencies more timely and efficient, public health laboratory modernization, bioterrorism preparedness, and programs to support mental health and prevent suicide and substance misuse. These cuts won’t only be felt in Washington, DC, or Atlanta—the Texas Department of State Health Services is losing nearly $877 million in funding, including staff and laboratories that are critical to its measles response. The Arkansas Department of Health, Human Services, and Education reports that it lost over $179 million in federal funding. Colorado reports losing more than $230 million, Illinois reports losing more than $400 million, Michigan reports losing more than $390 million, and Minnesota will lose approximately $200 million.
TFAH is dedicated to improving the nation’s health. The Administration’s goal of lowering rates of chronic disease in the U.S. is an important one. We want to work with the Administration and Congress on implementing evidence-based solutions to preventing and addressing chronic disease and other health challenges facing the country, as outlined in our Blueprint for Strengthening Public Health for the New Administration and Congress report. Our immediate appeal to federal policymakers, including Secretary Kennedy, is to not dismantle the nation’s health promotion infrastructure without careful review and input from Congress and health experts on how to make systems more effective and efficient while also adhering to the foundational ethos of medicine: first, do no harm.
Trust for America’s Health is a nonprofit, nonpartisan public health policy, research, and advocacy organization that promotes optimal health for every person and community and makes the prevention of illness and injury a national priority.
New Report Measures States’ Preparedness for Public Health Emergencies, Including Infectious Disease Outbreaks and Extreme Weather Events
Special Feature Examines the Threat of H5N1 Bird Flu and How to Guard Against Its Spread
(Washington, DC – March 27, 2025) – A new report assessing national and state preparedness to protect residents’ health during emergencies found that 29 states placed in the middle or low-performance tier for emergency preparedness, and that all states can do more to strengthen their readiness.
During 2024, the nation experienced a significant number of public health emergencies, ranging from infectious disease outbreaks to weather-related disasters. These emergencies demonstrate the urgent need for sustained investment in public health infrastructure and emergency preparedness, both of which are critical to the nation’s overall health and national and economic security.
Ready or Not 2025: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism, released today by Trust for America’s Health (TFAH), measures states’ readiness for a range of health emergencies based on 10 indicators, including healthcare system readiness, state public health funding, public health laboratory surge capacity, employee access to paid time off, and community water system safety.
The report, now in its 22nd year of publication, places states and the District of Columbia into three performance tiers for emergency preparedness. This year’s report placed 21 states and DC in the high-performance tier, 16 states in the middle-performance tier, and 13 states in the low-performance tier.
| Table 2: State Public Health Emergency Preparedness State Performance, by scoring tier, 2024 |
||
| Performance Tier | States | Number of States |
| High Tier | CO, CT, DC, DE, FL, GA, ID, MA, MD, ME, MO, NC, NH, NJ, OH, PA, RI, UT, VA, VT, WA, WI | 21 states and DC |
| Medium Tier | AL, AR, AZ, CA, IA, IL, IN, KS, KY, ND, NE, NY, OK, SC, TN, TX | 16 states |
| Low Tier | AK, HI, LA, MI, MN, MS, MT, NV, NM, OR, SD, WV, WY | 13 states |
The report provides federal, state, and local policymakers and health officials with benchmarks and policy recommendations that outline how jurisdictions can strengthen their emergency preparedness.
“Strengthening communities for public health emergencies requires sustained investment, planning, and multi-sector cooperation,” said J. Nadine Gracia, M.D., MSCE, President and CEO of Trust for America’s Health. “Recent public health emergencies, from measles and tuberculosis outbreaks to wildfires and extreme heat, demonstrate the need for consistent investment in public health infrastructure and workforce and programs that support health in every community – because a healthy community will be more resilient when emergencies happen.”
The report includes a special feature on H5N1 bird flu, including recommendations from public health experts on steps the country should take to protect against the outbreak evolving into a pandemic. The feature discusses the importance of extensive testing programs and collaborative efforts including ways in which public health officials are working with partners in the agriculture and veterinary medicine sectors to control the outbreak.
New to the report this year is a performance indicator measuring avoidable mortality—deaths caused by preventable or treatable conditions. This indicator measures deaths before age 75 that could be prevented through effective public health measures or averted with timely healthcare interventions. Higher rates of avoidable mortality indicate gaps in public health and healthcare systems, which can weaken a community’s ability to respond to and recover from public health emergencies.
Overall, the report finds areas of strength and areas for improvement.
Areas of strong performance include:
- Nurse Licensure Compact: More states have adopted the nurse licensure compact that allows nurses to work in any member state with a single multistate license. The compact is a tool for enabling healthcare facilities to surge nursing staff during an emergency. As of January 2025, 41 states belong to the nurse licensure compact, an increase from the previous year.
- Public Health and Emergency Management Accreditation: Most states have achieved accreditation through the Public Health Accreditation Board (PHAB) and/or the Emergency Management Accreditation Program (EMAP). Accreditation helps agencies strengthen emergency readiness by fostering continuous improvement, establishing clear governance structures, and enhancing coordination. Accredited states also benefit from well-defined processes and robust monitoring and evaluation systems—key factors in effectively responding to public health emergencies and disasters.
- Water Safety: In most states, 95 percent of households get their water from a municipal water system that did not have any water safety violations.
Areas for improvement include:
- Avoidable Mortality: Avoidable mortality—deaths from preventable or treatable causes—varies widely across the country, reflecting differences in healthcare access, public health infrastructure, and underlying social and economic factors. Some states have significantly lower rates of avoidable deaths, while others face persistently high burdens. Geographic disparities are evident, with avoidable mortality rates highest in parts of the Southeast and Appalachia. Some states in the Great Plains and Mountain West also experience high rates. In contrast, states in the Northeast and Upper Midwest generally have lower rates. Additionally, Black and American Indian/Alaska Native populations frequently experience the highest rates of avoidable deaths, often due to barriers to good health within their communities. These disparities underscore the importance of ensuring that all residents have access to effective public health and healthcare services.
- State Public Health Funding: Fourteen states reduced public health funding in FY 2024, three more than the eleven that reduced funding in FY 2023. The reduction may be related to the loss of COVID-19 response funding but is important to track particularly as states are also facing reductions in federal health and emergency preparedness funding.
- Limited Access to Paid Time Off: On average, only about half of workers in each state used some form of paid time off during a given month. Access to paid time off allows people to avoid spreading illness in the workplace. Employers who provide employees with paid sick leave are not only helping to control the spread of infections within their community, they are also supporting their business stability and helping to safeguard the local economy.
- Low Flu Vaccination Rates: Too few people are vaccinated against seasonal flu. During the 2023 – 2024 flu season only 47 percent of the population (ages six months and older) were vaccinated against the flu, down from the previous year and well short of the 70 percent goal established by Healthy People 2030. Improving flu vaccination rates can protect health, particularly for people at higher risk of serious flu outcomes and can reduce demand on the healthcare system. Improved rates also help guard against the potential for significant economic toll of a severe flu outbreak due to higher healthcare costs and lost business productivity.
Recommendations for Improving Emergency Preparedness:
- Provide stable, sufficient funding for public health capabilities, including Centers for Disease Control and Prevention’s (CDC) public health emergency preparedness funds that go to states, territories, and localities, and continue to modernize health data systems to improve detection of new threats.
- Reauthorize the Pandemic and All-Hazards Preparedness Act (PAHPA) to improve the nation’s readiness to manage a spectrum of health threats.
- Prevent and respond to infectious disease threats by funding CDC’s National Immunization Program and Antimicrobial Resistance Solutions Initiative.
- Reduce health disparities in the impact of emergencies by improving demographic data collection and reporting and by targeting health investments where they are most needed. Community readiness can also be improved by engaging populations that are disproportionately impacted into the emergency planning process.
- Accelerate the development and stockpiling of vaccines, therapeutic medicine, and diagnostic testing for faster distribution during emergencies.
- Ensure healthcare system readiness through increased cross-state credentialing for nurses and other healthcare professionals and by fortifying the Administration for Strategic Preparedness and Response’s Health Care Readiness program.
- Expand and fully fund CDC’s initiatives to address extreme weather and other environmental threats.
Read the full report
Trust for America’s Health is a nonprofit, nonpartisan public health policy, research, and advocacy organization that promotes optimal health for every person and community and makes the prevention of illness and injury a national priority.
Un nuevo informe mide la preparación de los estados ante emergencias de salud pública, incluidos brotes de enfermedades infecciosas y fenómenos meteorológicos extremos
Un artículo especial examina la amenaza de la gripe aviar H5N1 y cómo protegerse contra su propagación
(Washington, DC, 27 de marzo de 2025): Un nuevo informe que evalúa la preparación nacional y estatal para proteger la salud de los residentes durante emergencias ha revelado que 29 estados se sitúan en un nivel medio o bajo de rendimiento en cuanto a preparación ante emergencias, y que todos los estados pueden hacer más para reforzar su preparación.
Durante 2024, el país experimentó un número significativo de emergencias de salud pública, desde brotes de enfermedades infecciosas hasta desastres climáticos. Estas emergencias demuestran la urgente necesidad de una inversión sostenida en infraestructura de salud pública y preparación para emergencias, ambos aspectos cruciales para la salud general y la seguridad nacional y económica del país.
Ready or Not 2025: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism, publicado hoy por Trust for America’s Health (TFAH), mide el nivel de preparación de los estados ante una variedad de emergencias sanitarias basándose en 10 indicadores, entre ellos, la preparación del sistema de salud, la financiación estatal de salud pública, la capacidad de los laboratorios de salud pública de responder ante emergencias, el acceso de los empleados a tiempo libre remunerado y la seguridad del sistema de agua comunitario.
El informe, que se publica desde hace 22 años, clasifica a los estados y al Distrito de Columbia en tres niveles de desempeño en materia de preparación ante emergencias. El informe de este año clasificó a 21 estados y al Distrito de Columbia en el nivel de alto desempeño; a 16 estados, en el nivel de desempeño medio; y a 13 estados, en el nivel de bajo desempeño.
Nivel de alto desempeño: 21 estados y el Distrito de Columbia
CO, CT, DC, DE, FL, GA, ID, MA, MD, ME, MO, NC, NH, NJ, OH, PA, RI, UT, VA, VT, WA, WI
Nivel de desempeño medio: 16 estados
AL, AR, AZ, CA, IA, IL, IN, KS, KY, ND, NE, NY, OK, SC, TN, TX
Nivel de bajo desempeño: 13 estados
AK, HI, LA, MI, MN, MS, MT, NV, NM, OR, SD, WV, WY
El informe ofrece a los responsables de formular políticas y a los funcionarios de salud federales, estatales y locales parámetros de referencia y recomendaciones de políticas que delinean cómo las jurisdicciones pueden fortalecer su preparación para emergencias.
“Fortalecer a las comunidades en situaciones de emergencia de salud pública requiere de inversión sostenida, planificación y cooperación multisectorial”, afirmó la Dra. J. Nadine Gracia, máster en ciencias de epidemiología clínica, presidenta y directora ejecutiva de Trust for America’s Health. “Las recientes emergencias de salud pública, desde brotes de sarampión y tuberculosis hasta incendios forestales y calor extremo, demuestran la necesidad de una inversión constante en infraestructura y personal de salud pública, así como en programas que apoyen la salud en todas las comunidades, ya que una comunidad sana será más resiliente cuando se presenten emergencias”.
El informe incluye un artículo especial sobre la gripe aviar H5N1, con recomendaciones de expertos en salud pública sobre las medidas que el país debería tomar para evitar que el brote se convierta en una pandemia. Este artículo analiza la importancia de los programas de pruebas exhaustivas y los esfuerzos de colaboración, incluidas las formas en que los funcionarios de salud pública están trabajando con socios en los sectores agrícola y veterinario para controlar el brote.
Una novedad en el informe de este año es un indicador de desempeño que mide la mortalidad evitable (muertes causadas por afecciones prevenibles o tratables). Este indicador mide las muertes antes de los 75 años que podrían prevenirse con medidas eficaces de salud pública o evitarse con intervenciones sanitarias oportunas. Tasas más altas de mortalidad evitable son indicativas de deficiencias en los sistemas de salud pública y de atención médica, lo que puede debilitar la capacidad de una comunidad de responder y recuperarse de las emergencias de salud pública.
En general, el informe identifica áreas de fortaleza y áreas de mejora.
Las áreas de desempeño destacado incluyen:
- Pacto para la licencia de enfermería: Más estados han adoptado el pacto para la licencia de enfermería, que permite a los enfermeros trabajar en cualquier estado miembro con una única licencia multiestatal. El pacto es una herramienta que permite a los centros de salud aumentar el personal de enfermería durante una emergencia. A partir de enero, 41 estados pertenecían al pacto para la licencia de enfermería, lo que representa un aumento respecto del año anterior.
- Acreditación en salud pública y gestión de emergencias: La mayoría de los estados han obtenido la acreditación a través de la Junta de Acreditación de Salud Pública (PHAB) o el Programa de Acreditación para la Gestión de Emergencias (EMAP). La acreditación ayuda a las agencias a fortalecer su preparación para emergencias, ya que promueve la mejora continua, establece estructuras de gobernanza claras y mejora la coordinación. Los estados acreditados también se benefician de procesos bien definidos y sistemas sólidos de monitoreo y evaluación —factores clave para responder eficazmente ante emergencias y desastres de salud pública.
- Seguridad del agua: En la mayoría de los estados, el 95 % de los hogares obtiene agua de un sistema municipal que no presenta ninguna infracción de seguridad hídrica.
Las áreas de mejora incluyen:
- Mortalidad evitable: La mortalidad evitable (muertes por causas prevenibles o tratables) varía ampliamente en todo el país, lo que refleja las diferencias en el acceso a la atención médica, la infraestructura de salud pública y los factores sociales y económicos subyacentes. Algunos estados tienen tasas significativamente más bajas de muertes evitables, mientras que otros enfrentan cargas persistentemente altas. Las disparidades geográficas son evidentes, con las tasas de mortalidad evitable más altas en partes del sureste y los Apalaches. Algunos estados de las Grandes Llanuras y las Montañas del Oeste también experimentan tasas altas. En cambio, los estados del noreste y el Alto Medio Oeste generalmente tienen tasas más bajas. Además, las poblaciones negras e indígenas estadounidenses/nativas de Alaska con frecuencia experimentan las tasas más altas de muertes evitables, a menudo debido a las barreras para acceder a una buena salud en sus comunidades. Estas disparidades subrayan la importancia de garantizar que todos los residentes tengan acceso a servicios de salud pública y atención médica eficaces.
- Financiamiento estatal de la salud pública: Catorce estados redujeron el financiamiento de la salud pública en el año fiscal 2024, tres más que los once que lo hicieron en el año fiscal 2023. Esta reducción puede estar relacionada con la pérdida de fondos para la respuesta al COVID-19, pero es importante hacer seguimiento de esto, especialmente porque los estados también enfrentan recortes en los fondos federales destinados a la salud y la preparación ante emergencias.
- Acceso limitado a tiempo libre remunerado: En promedio, solo la mitad de los trabajadores en cada estado utilizaron algún tipo de tiempo libre remunerado durante un mes determinado. El acceso a tiempo libre remunerado permite a las personas evitar la propagación de enfermedades en el lugar de trabajo. Los empleadores que ofrecen a sus empleados licencia por enfermedad remunerada no solo ayudan a controlar la propagación de infecciones en su comunidad, sino que también apoyan la estabilidad de su negocio y contribuyen a salvaguardar la economía local.
- Bajas tasas de vacunación contra la gripe: Muy pocas personas se vacunan contra la gripe estacional. Durante la temporada de gripe 2023-2024, solo el 47 % de la población (de seis meses o más) se vacunó contra la gripe, una cifra inferior a la del año anterior y muy por debajo del objetivo del 70 % establecido por Healthy People 2030. Mejorar las tasas de vacunación contra la gripe puede proteger la salud, en particular la de las personas con mayor riesgo de sufrir desenlaces graves a causa de la gripe, y puede reducir la demanda del sistema sanitario. Mejorar las tasas también ayuda a prevenir el posible impacto económico significativo de un brote grave de gripe debido al aumento de los costos de atención médica y la pérdida de productividad empresarial.
Recomendaciones para mejorar la preparación ante emergencias:
- Proporcionar financiación estable y suficiente para las capacidades de salud pública, incluidos los fondos de preparación para emergencias de salud pública de los Centros para el Control y la Prevención de Enfermedades (CDC) que se destinan a estados, territorios y localidades, y continuar modernizando los sistemas de datos de salud para mejorar la detección de nuevas amenazas.
- Reautorizar la Ley de Preparación para Pandemias y Todo Tipo de Peligros (PAHPA) con el fin de mejorar la preparación del país para gestionar diversas amenazas a la salud.
- Prevenir y responder a las amenazas de enfermedades infecciosas financiando el Programa Nacional de Inmunización y la Iniciativa de Soluciones para la Resistencia a los Antimicrobianos de los CDC.
- Reducir las disparidades de la salud en el impacto de las emergencias mejorando la recopilación y la presentación de datos demográficos y dirigiendo las inversiones en salud donde más se necesitan. La preparación comunitaria también puede mejorarse involucrando a las poblaciones que resultan afectadas de manera desproporcionada en el proceso de planificación para emergencias.
- Acelerar el desarrollo y el almacenamiento de vacunas, medicamentos terapéuticos y pruebas de diagnóstico para una distribución más rápida durante las emergencias.
- Garantizar la preparación del sistema de salud aumentando la acreditación interestatal de enfermeras y otros profesionales de la salud y fortaleciendo el programa de Preparación para la Atención Médica de la Administración de Preparación y Respuesta Estratégicas.
- Ampliar y financiar completamente las iniciativas de los CDC para abordar las amenazas climáticas extremas y otras amenazas ambientales.
Lea el informe completo
Trust for America’s Health es una organización de políticas de salud pública, investigación y defensoría sin fines de lucro y no partidista que promueve la salud óptima para todas las personas y comunidades, y hace de la prevención de enfermedades y lesiones una prioridad nacional.
Ready or Not 2025: Protecting the Public’s Health from Diseases, Disasters, and Bioterrorism
New National Adult Obesity Data Show Level Trend
Stabilization of Obesity Rates is Welcome News but More Investment in Prevention Policies and Programs is Needed
(Washington, DC – October 10, 2024) – Over the last two decades, obesity has increased across the country in both adults and children. Newly released National Health and Nutrition Examination Survey (NHANES) data from 2021–2023 find that 40.3 percent of adults had obesity, which is slightly lower than the previous data (2017–2020). This is tentatively positive news, as it suggests a possible stabilization of the overall adult obesity rates in the United States in recent years— though the rate is still much higher than prior decades.
Percent of Adults Ages 20 and Older with Obesity, 1999-2023
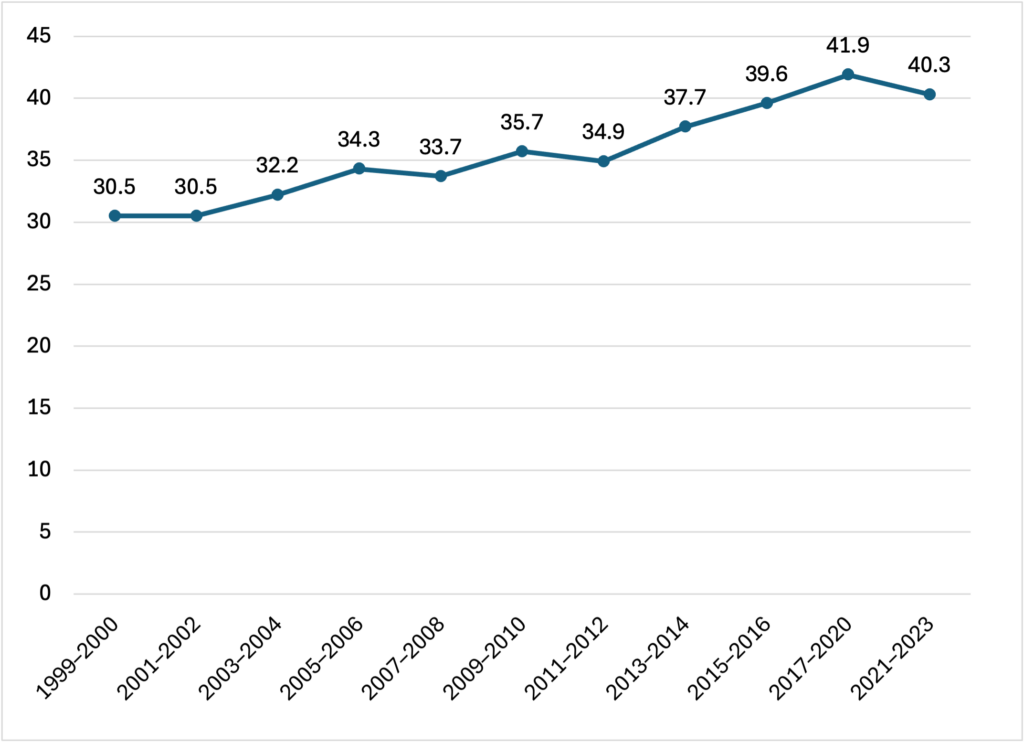
Source: NHANES
Obesity is a complex disease that is influenced by many factors beyond personal behavior. Reversing the nation’s obesity crisis requires sustained investment in multidimensional strategies and policies, that are tailored for population groups and regional differences. As TFAH’s September 2024 State of Obesity report explores, there are a number of evidence-based policies and programs that improve nutrition and support healthy eating, and help to reduce rates of obesity and chronic disease.
This includes important policy progress, like:
- Improving nutritional quality of the food supply and diets by prohibiting trans fats in foods, instituting voluntary guidance to reduce sodium in commercial foods, and taxing sugar sweetened beverages to reduce added sugar consumption.
- Empowering consumers through better labeling and education, like improved Nutrition Facts labels, new restaurant menu labeling, and family education programs.
- Increasing nutritional quality and access in schools, institutions, and nutrition programs, including aligning child nutrition programs and the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) with the Dietary Guidelines for Americans.
(See State of Obesity report pages 14–17 for more on these nutrition and food environment policies.)
Looking forward, we need to build on these initial steps to ensure that adult obesity rates continue to trend in the right direction, including critical policies like:
- Increase federal resources for evidence-based, effective efforts that reduce obesity-related disparities and related conditions including funding for CDC’s chronic disease and obesity prevention programs, such as the State Physical Activity and Nutrition, Racial and Ethnic Approaches to Community Health, and Healthy Tribes
- Decrease food and nutrition insecurity while improving the nutritional quality of available foods in every community by, among other activities, providing healthy school meals for all students and maintaining progress on the final 2024 school nutritional meal standards. In addition, Congress should expand access to nutrition support programs such as the Supplemental Nutrition Assistance Program (SNAP) and WIC, and increase the value of their benefits.
- To help consumers make informed choices, the Food and Drug Administration should swiftly implement a front-of-package label that will help people more easily understand the nutrients of concern in packaged foods.
(See State of Obesity 2024 recommendations on pages 67–76 for additional measures policymakers should take to continue to make progress in efforts to help all Americans maintain a healthy weight.)
“It is welcome news that the latest NHANES data suggest the overall adult obesity rate in this country has not been increasing in recent years,” said J. Nadine Gracia, M.D., MSCE, President and CEO of Trust for America’s Health. “However, much more needs to be done to address this health crisis. This is a critical moment to increase our efforts: boost and sustain investment in proven obesity prevention policies and programs and build healthier communities where everyone has access to affordable, nutritious foods and safe places to engage in physical activity.”
The new NHANES report also highlights the link between obesity and socioeconomic status. Like previous years, the new data show clear differences in obesity prevalence by educational attainment, with lower obesity rates for adults with a bachelor’s degree (31.6 percent) than in adults with less education (high school diploma or less (44.6 percent) and those with some college (45.0 percent). This underscores the critical role of policies and programs that boost accessibility and affordability of healthy food for all Americans.
Notably, the newly released report does not include data by race/ethnicity, though we hope that will be released later this year. Previous years’ data have shown large differences in obesity prevalence and trends by race/ethnicity. Understanding trends across different racial/ethnic groups, and if disparities are increasing or decreasing, is essential for a complete picture and successful policy response.
See TFAH’s State of Obesity 2024: Better Policies for a Healthier America report for more information about obesity rates and solutions.
Pathway to a Healthier America: A Blueprint for Strengthening Public Health for the New Administration and Congress
How Healthy People 2030 Has Led to Success Changing the Narrative on Healthy Aging
September is National Healthy Aging Month, and Trust for America’s Health (TFAH) is proud that its Age-Friendly Public Health Systems initiative (AFPHS) has led to state, local, and tribal efforts to help older adults remain active and independent and reframe the narrative around aging.
The AFPHS initiative aligns with National Healthy Aging Month and Healthy People 2030, a federal initiative that identifies public health priorities to help individuals, organizations, and communities across the United States improve health and well-being. The Office of Disease Prevention and Health Promotion (ODPHP) at the U.S. Department of Health and Human Services, in collaboration with a diverse group of partners and organizations, leads and manages the Healthy People initiative, which sets national objectives every 10 years. TFAH is honored to be officially recognized as a Healthy People 2030 Champion. The current iteration of the Healthy People initiative incorporates a variety of new objectives and targets for improving conditions for older adults. (See full list here).
Both Healthy People 2030 and TFAH’s AFPHS 6C’s Framework emphasize community partnerships and effective communication to meet the needs of older adults. Through the AFPHS initiative, TFAH has worked closely with federal partners to encourage and support collaboration between state, local, tribal, and territorial public health and aging agencies. Highlights from these collaborations include:
- A partnership in Hawai’i — the Kūpuna Collective — that supports age-inclusive ways to maximize health, independence, and engagement among older adults. Network members include foundations, nonprofit and community-based organizations, healthcare organizations, and academic institutions.
- Implementation of the Counseling on Access to Lethal Means (CALM) program by the Georgia Departments of Health and Aging Services to promote mental health among older adults and limit access to lethal means of suicide.
- A joint effort among tribal nations in Region 6 to provide training, resources, services, and funding for improving nutrition education and supplying meals.
Building an age-friendly ecosystem that holistically supports healthy aging should be a priority in communities across the country since nearly a quarter of the U.S. population is expected to be 65 years or older by 2060.
TFAH co-hosted the National Healthy Aging Symposium with ODPHP on September 26, 2024 to elevate successful innovations that improve older adult health and well-being and provide a forum to learn from experts in fields like brain health, caregiving, and social determinants of health.
The National Healthy Aging Symposium
Nuevo informe: La obesidad adulta en EE. UU. alcanza niveles epidémicos
Las tasas de obesidad son predominantemente más elevadas en las comunidades que experimentan obstáculos para una alimentación sana y en las que tienen pocas oportunidades para la actividad física.
(Washington, DC – 12 de septiembre de 2024) – Según un informe publicado el día de hoy por Trust for America’s Health (TFAH, por sus siglas en inglés.) Las tasas de obesidad entre los adultos estadounidenses eran iguales o superiores al 35% en veintitrés estados en 2023, lo que representa un aumento de varias décadas en las tasas de estadounidenses que viven con obesidad. En 2012, ningún estado tenía una tasa de obesidad en adultos igual o superior al 35%.
El informe Estado de la obesidad 2024: Mejores políticas para una America más saludable, incluye el análisis de TFAH de los datos más recientes del Sistema de Vigilancia de Factores de Riesgo del Comportamientos (BRFSS) de los Centros para el Control y la Prevención de Enfermedades (CDC). La obesidad y otras enfermedades relacionadas con la dieta se asocian a una serie de afecciones físicas y mentales, mayor mortalidad, mayores costos sanitarios y pérdidas de productividad.
Los estados con las tasas más altas de obesidad entre los adultos en 2023 fueron Virginia Occidental (41,2 por ciento), Misisipi (40,1 por ciento), Arkansas (40,0 por ciento), Luisiana (39,9 por ciento) y Alabama (39,2 por ciento). Entre 2022 y 2023, tres estados experimentaron aumentos estadísticamente significativos en sus tasas de obesidad adulta: Alaska, Arkansas y Oregón, mientras que ningún estado tuvo un descenso estadísticamente significativo. Entre 2018 y 2023, 28 estados experimentaron aumentos estadísticamente significativos en las tasas de obesidad adulta.
Los estados con niveles más bajos de obesidad adulta en 2023 fueron el Distrito de Columbia (23,5 por ciento), Colorado (24,9 por ciento), Hawai (26,1 por ciento), Massachusetts (27,4 por ciento) y California (27,7 por ciento).
A nivel nacional, más de cuatro de cada diez adultos estadounidenses padecen de obesidad. Aunque las tasas de obesidad han aumentado en todos los grupos de la población, los grupos con las tasas más altas son con frecuencia las poblaciones de color, ya que enfrentan obstáculos a nivel de estructura para lograr una alimentación sana, algunas de estas limitaciones incluyen, el costo, acceso a los alimentos, la falta de oportunidades y lugares para realizar actividad física. Los adultos negros y latinos y las personas que viven en comunidades rurales tienden a tener las tasas más altas de obesidad.
Las tasas de obesidad también están aumentando entre niños y adolescentes, casi el 20% de los niños y adolescentes estadounidenses entre 2 y 19 años padecen obesidad. Estas tasas se han más que triplicado desde mediados de la década de 1970, los jóvenes negros y latinos tienen tasas de obesidad sustancialmente más elevadas en comparación con sus pares blancos.
Una sección especial del informe analiza el entorno alimentario del país y los factores que afectan al consumo de alimentos, como las políticas alimentarias, la oferta, el suministro, el acceso y los precios, así como la influencia de la publicidad de alimentos en lo que la gente consume. La sección analiza las oportunidades que tienen los responsables políticos para hacer que el entorno alimentario sea más propicio para una alimentación sana, especialmente en las comunidades con bajos ingresos.
“El número de personas que viven con obesidad y las tasas de enfermedades relacionadas con la obesidad siguen aumentando, por lo que urge dar respuestas políticas a nivel sistémico”, ha declarado la Dra. J. Nadine Gracia, MSCE, presidenta y directora general de Trust for America’s Health. “La epidemia de la obesidad no se debe únicamente al comportamiento individual, sino que también influyen factores socioeconómicos y ambientales que escapan en gran medida al control de cualquier persona. Los responsables políticos deben actuar para hacer frente a esta creciente crisis sanitaria.”
Se necesitan medidas políticas
El informe incluye recomendaciones políticas basadas en pruebas para funcionarios federales, estatales y locales, así como para otras partes interesadas, como el sector sanitario y la industria alimentaria. Entre las medidas políticas recomendadas se incluyen:
Aumentar los recursos federales para lograr reducir las disparidades relacionadas con la obesidad y las afecciones relacionadas, otorgando financiamiento para los programas de prevención de enfermedades crónicas y obesidad de los CDC, incluidos los programas estatales de Actividad Física y Nutrición, Enfoques Raciales y Étnicos para la Salud Comunitaria y Tribus Saludables.
Disminuir la inseguridad alimentaria y nutricional para mejorar la calidad nutricional de los alimentos disponibles en cada comunidad, entre otras actividades, proporcionando comidas escolares saludables para todos los estudiantes y manteniendo el progreso en las normas finales de comidas nutricionales escolares de 2024. Además, el Congreso debe ampliar el acceso a los programas de apoyo a la nutrición como el Programa de Asistencia Nutricional Suplementaria (SNAP) y el Programa Especial de Nutrición Suplementaria para Mujeres, Bebés y Niños (WIC) y aumentar el valor de sus beneficios.
Ayudar a los consumidores a elegir con conocimiento de causa, la Administración de Alimentos y Medicamentos debe implantar rápidamente una etiqueta en la parte frontal del envase que ayude a comprender de manera sencilla los nutrientes de los alimentos envasados.
Eliminar los vacíos tributarios y las deducciones de costos empresariales por la publicidad de alimentos y bebidas poco saludables dirigida a los niños. También puede fomentarse la elección de alimentos y bebidas saludables imponiendo impuestos a las bebidas azucaradas.
Garantizar que todas las comunidades dispongan de un entorno que fomente el transporte activo, por ejemplo, ir a pie o en bicicleta a los destinos cotidianos y de lugares seguros para realizar actividades físicas, como parques y otros lugares para jugar dentro y fuera de casa.
Los legisladores, la atención médica y la salud pública, entre otras partes interesadas, deberían lograr que el acceso a la atención sanitaria este al alcance de todos, expandiendo Medicaid y ofreciendo un buen mercado de salud que sea asequible para todos. Medicaid, Medicare y otros programas deberían cubrir los servicios relacionados con la obesidad sin que el paciente tenga que compartir los costos.
El Congreso debe abordar las causas que producen las enfermedades crónicas e incentivar la colaboración multisectorial para abordar los factores sociales y componentes ambientales que afectan la condición de salud, la atención medica y las aseguradoras deben continuar expandiendo estrategias para evaluar y reembolsar las necesidades sociales relacionadas con la salud de los pacientes.
Lea el informe completo
Trust for America’s Health es una organización no partidista y sin ánimo de lucro dedicada a la investigación, la política y la defensa de la salud pública, que promueve una salud óptima para todas las personas y comunidades y hace de la prevención de enfermedades y lesiones una prioridad nacional. www.tfah.org