State and local public health and preparedness programs will be significantly impacted
(Washington, DC – September 18, 2025) – Health departments in states and localities nationwide are facing severe budget reductions due to current and proposed federal cuts, funding clawbacks, layoffs and hiring freezes, and agency reorganizations. These actions will weaken the nation’s public health system and emergency readiness and response and will put the country’s health and economic security at risk. So concludes a new report, Public Health Infrastructure in Crisis: HHS Workforce Cuts, Reorganizations, and Funding Reductions: Impacts and Solutions released today by Trust for America’s Health (TFAH), a non-partisan, non-profit organization focused on public health research and policy.
The report, which includes original analysis by TFAH, tallies the impacts of budget and staff reductions and proposed agency reorganizations to date as well as additional proposed changes and highlights the following findings:
- The President’s proposed FY 2026 budget for the Centers for Disease Control and Prevention (CDC) amounts to a 53 percent reduction in funding as compared to FY 2024. This figure reflects proposed cuts to CDC and its sister agency, the Agency for Toxic Substances and Disease Registry (ATSDR). These reductions are pending Congressional action.
- In addition, within the total proposed cut, CDC’s Public Health Emergency Preparedness program faces a 52 percent funding reduction.
- Overall, the proposed budget cuts CDC and ATSDR funding by slightly more than half and then restores about one-quarter of the lost funding to two newly proposed HHS divisions: the Administration for a Healthy America and the Office of Strategy.
- Over 100 public health programs and funding lines would be eliminated under the President’s proposed FY 2026 budget including 61 programs at CDC and 40 programs at the Substance Abuse and Mental Health Services Administration. Programs facing elimination include cancer, diabetes, heart disease, and stroke prevention programs, obesity prevention programs, global and domestic HIV/AIDS prevention programs, global immunization programs, and opioid and other substance use prevention and recovery programs.
- The proposed reorganization of U.S. Department of Health and Human Services (HHS) agencies would reduce the number of staff positions working on public health programs by 16 percent, even when accounting for the creation of the proposed Administration for a Healthy America.
- This year’s termination of already-approved funds clawed back over $12 billion in COVID-19 era grants – funding that in addition to supporting the pandemic response was intended to strengthen public health infrastructure beyond the needs created by the pandemic, including infectious disease monitoring, laboratory capacity, emergency preparedness, and mental health services.
The report is focused on changes to CDC and other select HHS agencies due to their central role in supporting public health programs and crisis response at the state and local level. About 80 percent of the CDC’s domestic budget flows to states, localities, tribes and tribal organizations, healthcare systems, and community partners to support state and local public health initiatives. Federal funding accounts for about half of state and local health department budgets so cuts to federal spending are cuts to local public health budgets.
“The consequential changes occurring in federal public health agencies impact every community and the lives of every American. State and local health departments, which are on the frontlines of protecting the health of their residents rely on the federal government, particularly CDC, for public health funding, expertise, and technical assistance. With the loss of funding, workforce, and programs, our country will be less prepared for future health emergencies, Americans’ health will suffer, and healthcare costs will rise,” said J. Nadine Gracia, M.D., MSCE, President and CEO, Trust for America’s Health.
Included in the report are interviews with two public health officials – Dr. Scott Harris, State Health Officer of Alabama, and Dr. Katherine Wells, Director of Public Health, City of Lubbock, Texas – describing the on the ground impacts and challenges created by the recent and proposed federal actions. Both are grappling with budget reductions of at least half of their annual budget due to federal cuts.
The report also acknowledges that the public health system has room for improvement. It needs to be modernized and strengthened to meet ongoing and emerging population health challenges. The report calls for collaboration between the administration, Congress, and public health leaders to strengthen the system through data driven actions. Some of the policy actions it recommends are:
- Congress and the administration should restore federal health agencies, funding, and workforces that were cut in 2025.
- The administration and Congress should maintain and strengthen the structure and capabilities of federal health agencies, which have specific, complementary, and distinct roles and expertise in protecting the nation’s health.
- Congress, in collaboration with federal agencies and outside experts and partners, should lead a bipartisan, deliberative process of reviewing proposals for federal health agency restructuring or development of new agencies.
- Congress and the administration should strengthen CDC as a national, comprehensive public health agency with responsibilities across the detection, prevention, and mitigation of the leading causes of preventable death, illness, and injury.
- Federal agencies must spend all funds appropriated by Congress, as required by law, and the Office of Management and Budget should release full-year funds to agencies after enactment of appropriations legislation.
- Congress should ensure continuous improvement of the nation’s public health capabilities and essential services, including workforces, laboratories, and data systems at all levels.
- Congress should restore the Prevention and Public Health Fund, a critical source of sustained funding for disease prevention and health promotion activities in every state and territory, as well as in localities and tribal communities, and prevent future cuts.




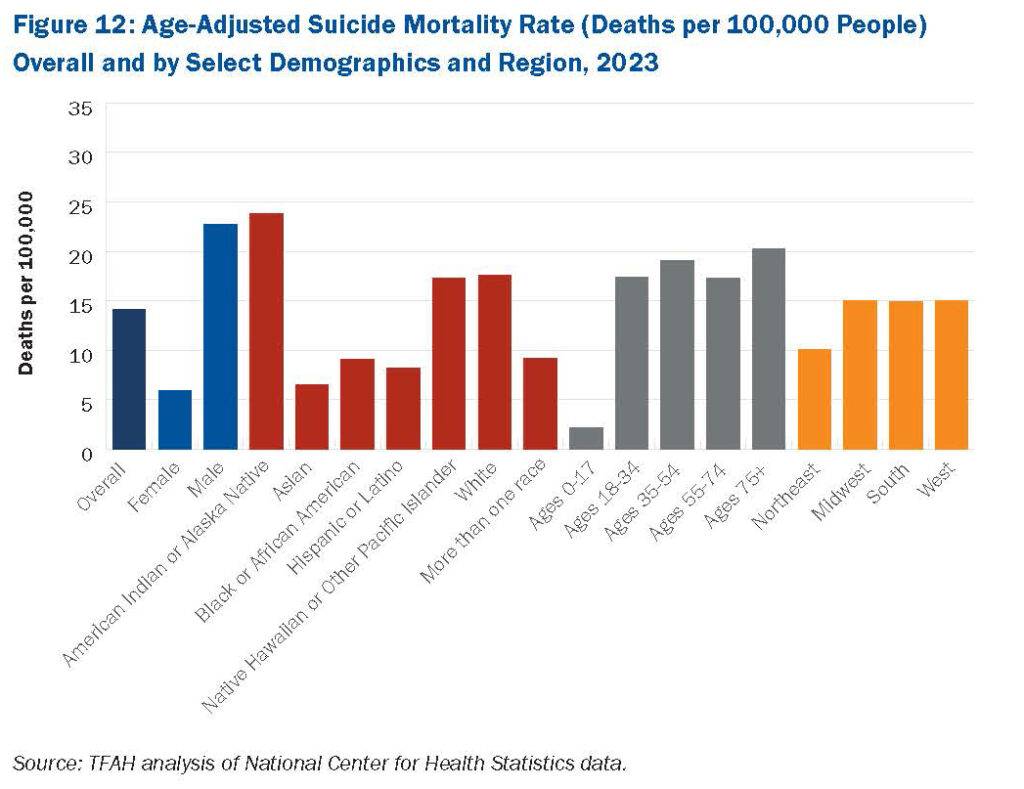 According to the latest edition of Trust for America’s Health’s
According to the latest edition of Trust for America’s Health’s 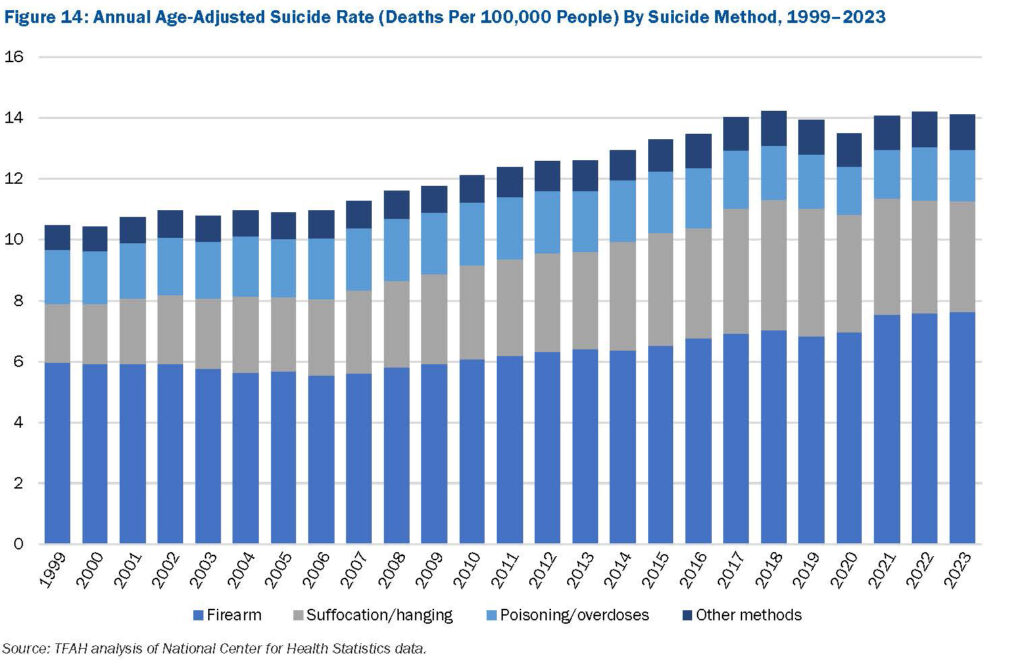 Some of the highest age-adjusted suicide rates are seen in males and adults ages 75 and older. Suicide rates in
Some of the highest age-adjusted suicide rates are seen in males and adults ages 75 and older. Suicide rates in 
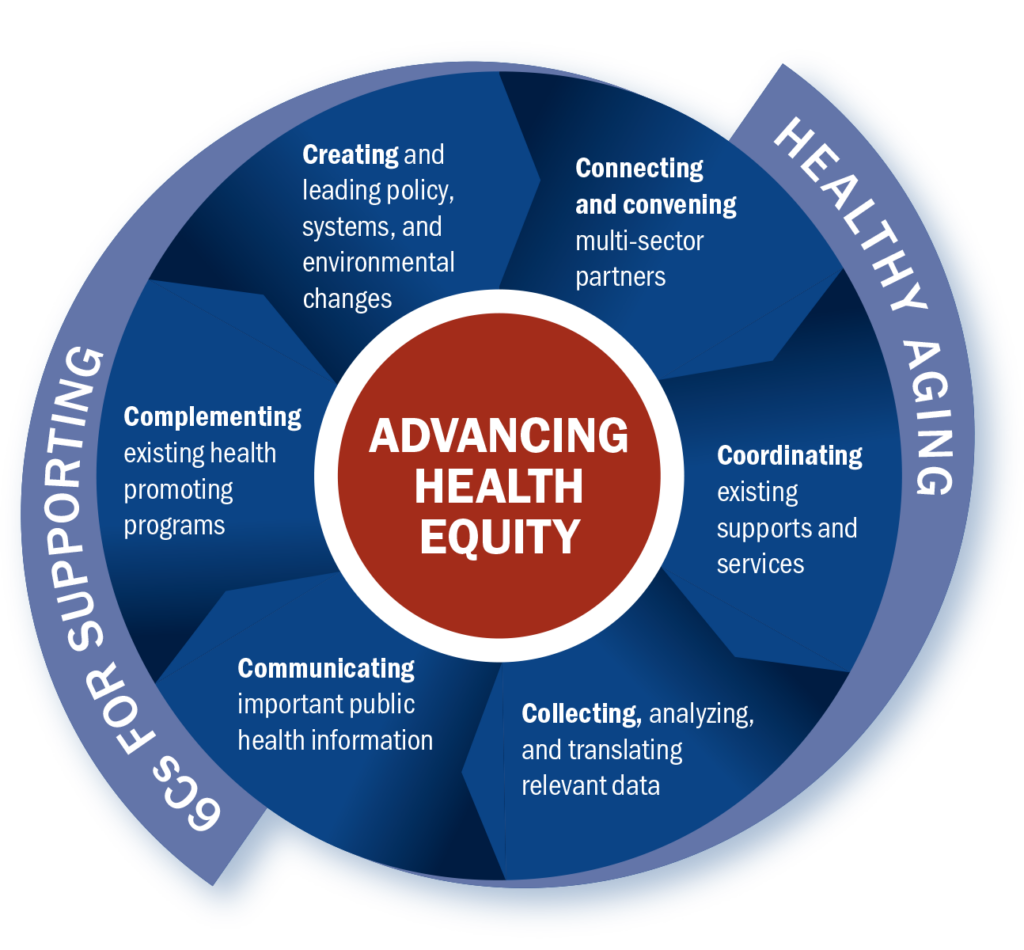 Megan: The Guide can be used by anyone who wants to build expertise in healthy aging, especially from a public health perspective. Our vision is that entire health department staffs will use it, but it’s also perfect for individuals or small teams to work through together.
Megan: The Guide can be used by anyone who wants to build expertise in healthy aging, especially from a public health perspective. Our vision is that entire health department staffs will use it, but it’s also perfect for individuals or small teams to work through together.