How can progress be sustained and extended to all communities?
(Washington, D.C. – May 28, 2025) – Deaths due to drug overdose and alcohol misuse were down in the United States in 2023 according to Centers for Disease Control and Prevention (CDC) data and newly released CDC 2024 provisional data predict an unprecedented 27 percent one year drop in overdose deaths. These reductions are encouraging and were likely related to a number of factors including investments in primary prevention, mental health, harm reduction, and overdose prevention programs. However, current and proposed federal budget cuts, public health workforce reductions, and proposed federal agency reorganizations are likely to undermine this progress, according to a new report.
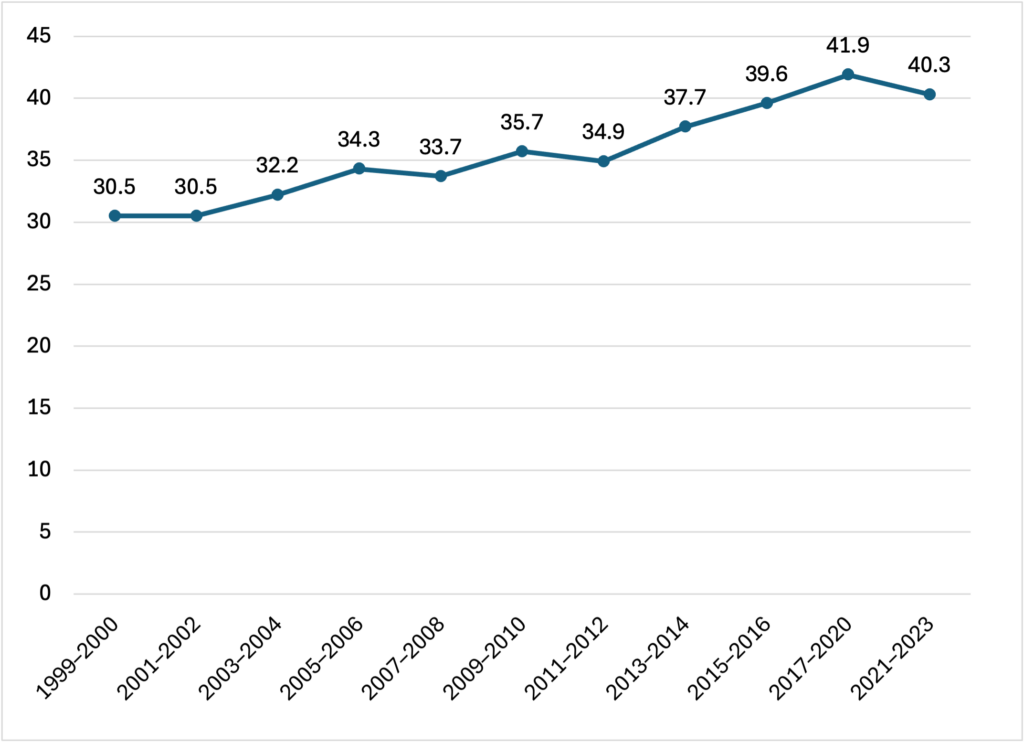
Pain in the Nation 2025: The Epidemics of Alcohol, Drug, and Suicide Deaths, released today by Trust for America’s Health, reports that the combined number of deaths from alcohol, drugs, and suicide in the United States declined in 2023 for the second straight year—after two decades in which such deaths increased at an alarming pace. Still over 200,000 Americans died due to alcohol, drug overdose, or suicide in 2023, twice the rate of such deaths 20 years ago.
The new data highlight the value of investment in mental health and substance use prevention programs – such as ensuring adequate mental health, substance use disorder, and crisis intervention services, access to overdose reversal drugs, and investing in children’s mental health and resilience. The data however also show that much more needs to be done to ensure that the progress against alcohol, drug overdose, and suicide deaths is sustained and that reductions in such deaths are occurring in every community and among all population groups.
“Data show that decades of investment and capacity building in substance use prevention, harm reduction programs, and mental health services have helped reduce associated deaths. The challenge now is to build on these investments and sustain this progress. These programs save lives; their funding should not be cut,” said J. Nadine Gracia, M.D., MSCE, President and CEO of Trust for America’s Health.
Drug overdose rates are declining but still at tragic levels.
In 2023, 105,007 Americans across died from drug overdoses. After precipitous increases in the rate of drug overdose deaths in 2020 and 2021, the 2022 overall overdose mortality rate was virtually unchanged and the 2023 mortality rate was 4 percent lower. Provisional mortality data for 2024 show an unprecedented one-year 27 percent decrease in overdose deaths nationally. Seven states (Louisiana, Michigan, New Hampshire, Ohio, Virginia, West Virginia, and Wisconsin) and Washington D.C. saw the greatest reductions, with declines of 35 percent or more in overdose deaths for the year.
According to public health experts, improved data systems which allow for real-time tracking of substance use and its impacts, the expansion and effectiveness of overdose prevention strategies such as programs to ensure access to naloxone, buprenorphine, and drug-checking tools all played a significant role in bringing down mortality rates.
The improvement was, however, not consistent across all population groups or regions of the country. In 2023, white people were the only racial/ethnic population group that experienced a statistically significant decrease in drug overdose deaths; other population groups had nonsignificant changes or increases. Drug overdose death rates in 2023 were highest among American Indian/Alaska Native people (AI/AN) (65.0 deaths per 100,000 people), adults ages 35 to 54 (57.3 deaths per 100,000 people), Black people (48.5 deaths per 100,000 people), and males (45.6 deaths per 100,000 people).
Alcohol-induced deaths are down.
In 2023, 47,938 Americans died from alcohol-induced causes. The overall age-adjusted alcohol-induced mortality rate decreased by 7 percent from 2022 to 2023 (from 13.5 to 12.6 deaths per 100,000 people). This decrease built on a 6 percent reduction the year prior and crossed nearly all demographic and geographic groups, but such deaths still disproportionately impact some groups. Alcohol-induced death rates in 2023 were highest among AI/AN people (61.5 deaths per 100,000 people), adults ages 55 to 74 (32.5 deaths per 100,000 people), adults ages 35 to 54 (20.2 deaths per 100,000 people), and males (18.1 deaths per 100,000 people).
Suicide deaths unchanged.
The U.S. overall suicide mortality rate remained virtually identical from 2022 to 2023 (14.2 and 14.1 deaths per 100,000 people, respectively). In 2023, 49,316 Americans died from suicide. Age-adjusted suicide rates in 2023 were highest among AI/AN people (23.8 deaths per 100,000 people), males (22.7 deaths per 100,000 people), and adults ages 75 and older (20.3 deaths per 100,000 people).
Budget rescissions and future cuts to prevention programs will cost lives.
While these data demonstrate real progress, the public health community is united in its concern about progress reversals due to cutbacks in federal investment in health promotion, crisis intervention, and overdose prevention programs. For example, staff and funding for the CDC Injury Center have been drastically reduced, and the Center is proposed for elimination in the Administration’s budget request for fiscal year (FY) 2026. The Injury Center conducts research and collects data. Approximately 80 percent of its funding goes to states and other entities for prevention of overdoses, suicide, and adverse childhood experiences (ACEs). Additionally, the Substance Abuse and Mental Health Services Administration (SAMHSA) has experienced major staffing reductions including staff working on the 988 Suicide & Crisis Lifeline, and a potential $1.07 billion funding cut for FY 2026. The Administration has proposed folding some remaining SAMHSA and Injury Center programs into a new Administration for a Healthy America. These actions followed the Administration’s claw-back of billions of dollars in public health funding already at work in states and communities across the country, including for suicide prevention.
The Pain in the Nation report calls for sustained investment in prevention and harm reduction programs and includes recommendations on actions federal and state policymakers should take including:
- Protect and bolster investment in public health and behavioral health systems and injury and violence prevention programs to improve mental health and well-being for all Americans.
- Continue to improve programs, like CDC’s Overdose Data to Action, to track emerging trends by geographic, demographic, and drug type metrics to guide local, state, and national responses and to prevent overdoses and deaths in real time.
- Focus on underlying drivers of substance use disorder through early intervention and prevention policies including expanding resiliency and substance use prevention programs in schools and increasing access to social and mental health services for children and families.
- Maximize harm reduction strategies and substance use disorder treatments to reduce overdose risk, and support efforts to limit access to lethal means of suicide.
- Bolster the continuum of crisis intervention programs and expand the mental health and substance use treatment workforce. Build community capacity to ensure access to mental health and substance use treatment for anyone needing such services.
Read the full report
Trust for America’s Health is a nonprofit, nonpartisan public health policy, research, and advocacy organization that promotes optimal health for every person and community and makes the prevention of illness and injury a national priority.